Patient of the Month- Evan W.
If you would like to make a donation to Soft Bones in honor of Evan, please click the button below!
My husband Will and I were excited and extremely nervous when we found out we were going to become first time parents. I had a pretty textbook pregnancy other than being diagnosed with gestational diabetes and a visit to a maternal fetal medicine doctor when our ultrasound tech noticed that Evan’s femur bone was measuring a little smaller than normal. The MFM specialist reported that Evan just had “short bones” and that “all of his bones were very white with no holes in them.” She said she didn’t see any complications and that we didn’t need to follow back up with her.
Evan was not a very active baby during my pregnancy. He would push on my ribs a lot but didn’t kick much. The day of my 35th week appointment with my OBGYN mentioned that Evan felt very low and that it was hurting to stand up. At this time I was barely even one cm dilated and we scheduled my induction. When I got into bed that night around 9PM my water broke. We immediately drove to Christus Lake Area Hospital. I was checked and was 1 cm dilated. The nurse told me and my husband to get comfortable and that we were in for a long night. To everyone’s surprise it was a quick, easy delivery! At 4am on November 23, 2022 Evan Wright was born. He weighed 5lbs 7oz and was 18 ½ inches long. Evan was rushed to the NICU because he was having a hard time breathing independently and he was put on a ventilator.
At first, the doctors thought his breathing issues were because of his prematurity, but when Evan was about a month old he had 3 failed extubation attempts. This is when we learned that Evan had some underlying complications that were causing him not to breathe on his own. One of the things we learned is that his rib bones were very thin, almost non-existent. This meant his chest cavity (and his lungs) were very underdeveloped. At the time, the doctors suspected Evan had HPP but they were waiting for test results to confirm. While we waited Evan started receiving Strensiq. Strensiq is a prescription medicine used to treat HPP. It works by replacing the ALP enzyme (the enzyme your body needs to mineralize healthy bones). He was also given versed (a pain medication) because he had fractures in his arms. The respiratory therapist started him on two different breathing treatments to help break up the secretions in his lungs. At this point we decided it was best to transfer Evan to Texas Children’s Hospital so he could receive the specialized care necessary for his condition.
We arrived on January 2nd and immediately knew we made the right decision. We were welcomed by Evan’s new team of doctors and nurses and they spent that first night monitoring Evan’s breathing and getting to know him.
The next morning we met with all of his specialists (respiratory, geneticist, dietician, Neonatologist, ENT, endocrinologist). We found out Evan has multiple fractures all over his body likely due to the trauma of delivery. Because of these multiple fractures they started giving him morphine and versed every 4 hours to keep him comfortable. He was officially diagnosed with Perinatal HPP January 12th at one month old.
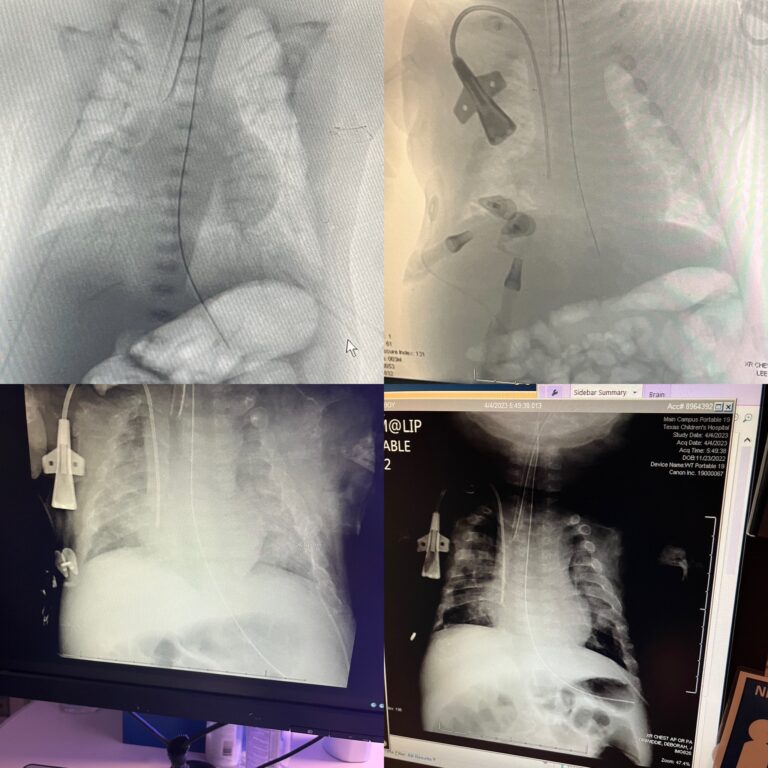
Because Evan was having to receive multiple blood transfusions and was on regular pain medicine his team thought it would be best to put in a central line. Evan hasn’t received a blood transfusion since February but he is still on his pain medications. On January 30th we received the amazing news that the Strensiq is WORKING! We saw a huge spike in his parathyroid hormone and his bones are continuing to calcify and growing stronger. (See x-ray from January, February, March, and April.) Evan is currently in physical therapy three times a week and has been able to sit up with assistance for about 15 minutes.
At this point Evan’s team at Texas Children’s are in communication with a Strensiq specialist in DuPont. On March 8th we met with his team to discuss a tracheostomy and a g tube placement. At the meeting they decided it wasn’t the right time for Evan to undergo surgery because they wanted to give his bones more time on the medicine. According to the Strensiq specialist Evan should show significant improvement 6 months to one year of being on Strensiq.
Now that Evan’s chest cavity has started to expand both doctors thought it was time to start ventilator weaning, but after one week of lowering vent settings Evan had a set back and we had to go back up on all his vent settings.
On April 3rd we had another meeting with Evan’s team to discuss trach and g tube placement. Evan didn’t do well on the portable ventilator so they were unable to perform an MRI to get a closer look at his neck bones. One big question right now is if Evan will be able to withstand the hyper extension of his neck that is necessary for tracheotomy placement. Everyone is amazed at the improvement in Evan’s bones since being on Strensiq. Right now our focus is to wait and allow the medication to do its job.
One big factor going into the trach decision is Evan’s physical and cognitive development. The trach will allow us to take Evan home and he will be able to have more normal interactions if he is at home in a normal family setting than he is getting right now at the hospital.
Evan is 4 months old now and even under these very difficult circumstances he smiles at everyone who walks up to his bed. We continue to pray that he will be able to get his tracheostomy soon so we can get him home.
I came across Soft Bones when searching for kids with HPP on Facebook. It has helped us a lot with reading other people’s journeys with HPP and strensiq. We are so thankful for this group because it has given us a lot of faith knowing Evan can still thrive in life. Everyone’s story is different but each and every one of you amaze us everyday.







Responses