Patient of the Month- Ashleigh F.

If you would like to donate to Soft Bones in honor of Ashleigh, please click the button below!

For most of my life, I knew something was wrong. As a child, I fractured my wrists three times—once on the left, twice on the right—and the very first time, both at once. Because of that, my mom never let me do gymnastics, which was all I ever wanted. For as long as I can remember, I’ve also dealt with dental issues. In my late 20s, I was diagnosed with celiac disease, which explained part of the puzzle: affecting enamel development, mineralization, and overall dental health due to nutrient malabsorption, a disorder where the small intestine cannot properly absorb nutrients, vitamins, and minerals from food. Going gluten-free slowed the progression, which was a relief, but it didn’t stop the issues entirely. With hypophosphatasia (HPP) also directly affecting tooth structure, it created a “double hit” to my dental health. After countless cavities, multiple filling replacements, seven crowns, and six root canals (all due to persistent and unexplained sensitivity), dental health has remained an ongoing battle.
Even when I was younger, I felt it—deep down in my bones (pun intended)—that I was more fragile than most. I naturally avoided certain foods, especially gluten, long before my celiac diagnosis. Fatigue was constant. I slept more than most, napped after school, and was never drawn to sports. Piano lessons, tennis lessons, and even a hip-hop class came and went, but nothing stuck. Fatigue has honestly been my number one symptom throughout my life.
Around age 20, I was diagnosed with Hashimoto’s, a chronic autoimmune disorder. I stayed on top of my health, undergoing bloodwork every 3–6 months and consulting with multiple endocrinologists over the years. Several doctors noted my low alkaline phosphatase levels but dismissed them as a “trend” or something “normal.” It wasn’t normal—and that would later become key to my diagnosis.
The Mystery Flare
At age 32, strange sensations started in my left big toe—gradually worsening to severe pain and loss of mobility. Walking hurt and going on my tiptoes was unbearable. Soon, pain and swelling spread up my ankle, calf, and behind my knee.
This went on for two years. Some days, I could barely get out of bed. Simple touches, like a bedsheet brushing my toe, would bring tears. My gait changed to compensate, causing peroneal tendonitis, calf muscle atrophy, and chronic swelling. X-rays and MRIs repeatedly showed nothing.
Other flares popped up, too. I thought I had carpal tunnel or a severe bicep injury—but imaging showed nothing. My wrist to shoulder became immobile for 30 days, yet doctors still saw “nothing.” Over two years, I saw orthopedic surgeons, physical therapists, podiatrists, general practitioners, endocrinologists, a neurologist, and eventually a rheumatologist. Nothing quite made sense.


Physical therapy was traumatic. Scraping, needling, cupping, and shockwave therapy—all made things worse. I left appointments in more pain than I arrived, with no improvement—just more anxiety.
Even my toenails got involved. At times, both big toenails would stop growing entirely for weeks or months. One nail even looked like it might fall off, though I never lost it, thankfully! Looking back, it was all part of the HPP puzzle.
Diagnosis and Validation
Frustrated with no answers, I used Teladoc for an expert medical review. They advised me to see a rheumatologist. At the first visit, he noticed my consistently low alkaline phosphatase and ordered B6 plasma levels. That’s when he suggested I might have HPP. Genetic testing later confirmed that I had juvenile-onset HPP, and my B6 levels were extremely elevated.
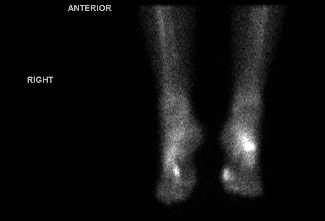
Finally, things made sense. One targeted MRI still showed nothing, but a nuclear bone scan lit up both feet—proof that my pain was real. The weight of being dismissed for years was finally lifted!
Treatment and Life Changes
Before treatment, unpredictability was the hardest part of living with HPP. I never knew when a flare would hit, where it would appear, or how long it would last—hours, days, weeks, or years. This taught me patience and compassion for my body in ways I never had before.
In 2023, stress at work peaked, and I realized I needed to prioritize my health. I quit my 9-to-5 after 11 years—a huge leap, but it opened the door to health and fitness coaching, helping women build sustainable habits and reclaim their confidence, while giving myself the much-needed chance to slow down and live at my own pace.
After nine months of fighting with insurance, I started Strensiq®, which has truly changed my life. The intense flares stopped. Symptoms, if they occur, are short-lived and usually tied to overuse. The injections are a challenge for me in many ways, but they’re predictable, unlike my pre-treatment flares.
Despite Strensiq’s refrigeration requirements, I’m grateful for modern technology that lets me maintain my health and avoid flares—even when I’m traveling. One of my biggest fears at diagnosis was that trips, domestic or international, would come to a halt. Now I can plan with confidence and still enjoy life to the best of my ability.


Lessons and Gratitude
HPP is more than a bone disease. It’s systemic, invisible, and unpredictable. It’s taught me awareness, patience, and self-compassion. I still have limits, but I’ve learned to work within them, remaining strong and consistent in my health and fitness.
I’m endlessly grateful for my husband, who supports me every step of the way—from emotional support to helping with injections. And the Soft Bones community has been invaluable—especially early on, connecting me with people who truly understand what living with HPP feels like. I’m especially excited to attend my first National Patient Meeting this year. Being able to connect in person, learn, and share experiences with others who understand this rare condition—it truly feels like a luxury.
This journey hasn’t been easy, but finally having answers, treatment, and support has made all the difference. And for that, I am forever grateful.








Responses