A Mental Health Guide
for Hypophosphatasia
(HPP) Patients
A Resource for Therapists
A Resource
for Therapists

 How to Use This Guide
How to Use This Guide
This guide is intended to support mental health professionals in developing a foundational understanding of hypophosphatasia (HPP)—a rare, inherited, multisystem metabolic bone disease—and in contextualizing the psychological and emotional experiences of individuals and families affected by the condition. Although HPP is often defined by its physical manifestations, including pain, fatigue, fractures, mobility limitations, dental complications, and treatment burden, its mental health impact is substantial, complex, and frequently underrecognized.
Clinicians are encouraged to approach HPP using a biopsychosocial framework, recognizing that psychological distress in this population often reflects the cumulative effects of chronic physical symptoms, functional impairment, uncertainty, and repeated disruptions to daily life, roles, and identity. Presentations such as depression, anxiety, trauma-related symptoms, ambiguous grief, and shame may represent adaptive responses to prolonged illness burden and unpredictability rather than discrete psychiatric pathology. Effective care therefore requires careful differentiation between primary mental health conditions and distress that is intrinsically linked to physical disease processes and lived experience.
It is also important for therapists to understand that the scientific and clinical understanding of HPP continues to evolve. Research is advancing rapidly, yet gaps remain between emerging evidence, clinical practice, and patient-reported experiences. As a result, individuals with HPP may encounter discrepancies between their lived symptoms and what is reflected in the medical literature or acknowledged by healthcare providers. This disconnect can contribute to experiences of invalidation or gaslighting, even in the absence of malicious intent. Clinicians should recognize that many medical providers may lack comprehensive or up-to-date knowledge of rare diseases such as HPP, which can further complicate the clinical experience for patients and amplify psychological distress.

 This guide is designed to assist mental health professionals in:
This guide is designed to assist mental health professionals in:
- Situating mental health symptoms within the broader context of chronic, rare physical illness
- Recognizing the psychological consequences of diagnostic uncertainty, symptom invisibility, and systemic barriers to care
- Validating patient experiences while acknowledging the limitations of current medical knowledge
- Supporting individuals and families as they navigate identity, relationships, and meaning in the context of a lifelong condition
- By grounding therapeutic work in an informed, nuanced understanding of HPP and its psychosocial implications, clinicians can provide care that is both clinically rigorous and deeply validating—addressing not only symptom management, but also trust, resilience, and long-term psychological well-being.


 HPP Challenges Across the Lifespan
HPP Challenges Across the Lifespan
HPP presents different challenges across the lifespan, and because the spectrum of disease and severity varies, each individual’s experience is unique. The challenges patients and families face often evolve with age and stage of life. Below are examples of experiences that individuals with HPP and their caregivers may encounter. This list is not exhaustive, and no two journeys are exactly the same.

Children
- Frequent medical appointments with a variety of specialists
- Difficulty keeping up with peers physically due to muscle weakness, bone pain, fatigue, or fractures
- Delayed gross motor milestones or a waddling gait
- Early tooth loss of deciduous teeth may lead to speech and eating difficulties, as well as confidence issues
- Chronic pain that may be difficult to articulate, sometimes presenting as behavioral challenges or acting out
- Self-consciousness about physical differences (gait, braces, mobility aids)
- Need for school accommodations or IEPs that do not fit traditional categories
- Feelings of frustration or isolation when they cannot participate fully in activities
- Needle phobia may occur in those on enzyme replacement therapy

Adolescants
- Body-consciousness about lipodystrophy, which can lead to scarring for patients on enzyme replacement therapy
- Inability to keep up with peers in sports, extracurricular activities, or social events can also impact the ability to gain employment
- Increased awareness of being “different,” which may impact self-esteem and mental health
- Low stamina and fatigue that may interfere with academics or social life
- Ongoing treatment burden (e.g., regular injections, monitoring, appointments); medication must be kept refrigerated, which can add to additional independence, such as camps, college transitions, etc.
- Anxiety about transition to independence and future limitations

Adults
- Chronic pain, fatigue, and/or brain fog that may affect daily functioning and the ability to work
- In serious cases, fractures doing mundane tasks (walking off a curb)
- Missing days of work due to medical appointments, surgeries, flare-ups, or recovery
- Delayed diagnosis and medical gaslighting by doctors lead to frustration and anxiety
- The ability to travel can be limited if on enzyme replacement therapy (refrigerated medication)
- Career limitations due to physical demands and insurance concerns
- Concerns of medical coverage of enzyme replacement therapy
- Challenges with self-advocating around disease-related workplace accommodations
- Emotional strain related to living with a chronic, progressive condition that can have an uncertain prognosis
- Navigating complex care coordination and insurance challenges
- Financial strain related to time off, medical costs, or disability leave

Caregivers
- Missing work for medical appointments, emergencies, or school meetings
- Navigating complex care coordination and insurance challenges
- Advocating for appropriate IEPs, 504 plans, or workplace modifications
- Emotional stress and uncertainty about disease progression
- Physical and mental exhaustion leading to caregiver burnout
- Limited career advancement due to caregiving demand
- Financial strain related to treatment, travel, and time away from work
- For parents, guilt about being a genetic carrier and contributing to a child’s medical condition
- Strain on partnerships or marriages
Because HPP affects each person differently, individualized support is essential at every stage of life. In addition, there are some other emotional concerns that many HPP patients share.
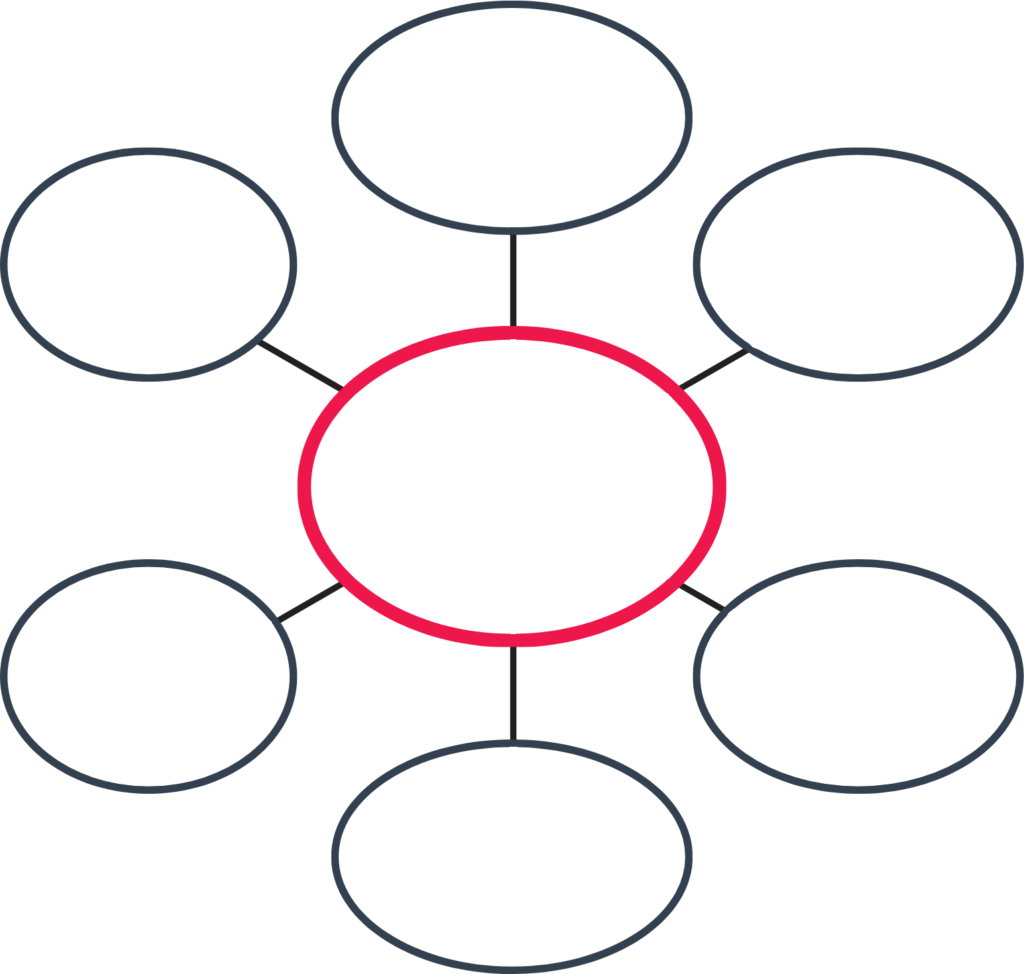
HPP and Potential
Impact on Mental Health
Financial
Stress
Inadequate
Medical Care
Mood &
Anxiety
Mental
Health
Stigma
Isolation
Physiological/
Neurological
 Mood/Anxiety
Mood/Anxiety
Depression: Change in activity levels, family and professional roles, chronic uncertainty, physical and emotional isolation
Quote: “It’s so hard never knowing how I am going to feel day to day.”
Anxiety: Impact of illness on ability to short-term and/or long-term plan for future, medical anxiety/white coat syndrome, treatment-related
Quote: “I worry every time I have to self-inject my medication.”
Acute/Chronic Trauma: experience/belief could die from illness, post-ICU syndrome (PICS), hypervigilance of symptoms (e.g., pain), negative experiences with the medical system
Quote: “So many doctors have misdiagnosed or dismissed me. It’s traumatizing to even walk into a doctor’s office sometimes.”
Ambiguous grief: Chronic nature of illness = unpredictable exacerbations and remissions
Quote: “Every time I think I have processed my health issues, something new happens, and I am grieving again.”
 Isolation
Isolation
Peer support: Lack of peers with specific diagnosis or rare disease
Quote: “Even people with other medical issues just do not understand what this is like.”
Interference with activities: Inability to participate in activities with family, friends, school, work; chronic unpredictability of ability to participate
Quote: “I never know how I am going to feel from one day to the next, even within the same day. I often end up being alone because I cannot commit to plans.”
 Stigma
Stigma
Invisible illness: Outside appearance does not indicate the level of symptoms, overall health, or disability. Pain, stamina, and post-surgical recovery.
Quote: “It constantly feels like I have to justify or defend my illness to people around me because I do not look sick. I cannot keep up with my friends; they think I’m not trying.”
Visible illness: Cranial shape, mobility devices, tracheotomy, synostosis, “Charlie Chaplin” gait
Quote: “People see my disability before they see me.”
Guilt/shame of “faulty” genes: Rare, inherited genetic mutation
Quote: “I inherited ‘bad’ genes and do not want to pass them on to future generations. Sometimes it feels like my genes are broken.”
 Psychological/Neurological
Psychological/Neurological
Pain: Headaches, muscle/joints, post-surgical, bone fractures
Sleep: Due to pain Medication side effects: anaphylaxis/hypersensitivity reactions, injection site reactions, fatigue, lipodystrophy
ADHD: higher comorbidity with HPP
Quote: “I am constantly having to manage my physical symptoms. I rarely/never just feel ok.”
 Financial Stress
Financial Stress
High financial burden: expensive medications, medical travel, adjunctive treatment costs, missing work/income, higher referral frequency, high-cost insurance plans
Quote: “Worrying about the expense of my illness is a constant stressor.”
 Inadequate Medical Care
Inadequate Medical Care
Misdiagnosis: Fibromyalgia, osteoporosis, MS, toll of being misdiagnosed, underdiagnosed, and dismissed for years
Lack of rare-specific providers: Very few doctors who treat HPP have to travel to find appropriate medical care from specialists
Lack of knowledge by general providers: Being more knowledgeable than the provider can be very uncomfortable
Quote: “Accurate diagnosis of a rare disease like HPP takes an average of 8-10 years. Even with a correct diagnosis, I have to be my own advocate 24/7 to receive appropriate care.”
This resource is sponsored in part by Alexion, AstraZeneca Rare Disease

